Parkinson’s disease is a progressive neurodegenerative disease, meaning that brain cells will continuously die off as the illness persists. The brain cells that are mainly affected in Parkinson’s disease are ones that produce dopamine, a chemical in the brain that is known to be important in the control of the body’s movement. What this translates to in terms of symptoms is a disease progression in which the patient’s ability to control movement worsens over time. Patients start off feeling a slight resting tremor, which progresses to rigidity, and loss of balance. In the advanced stages of the disease, the patient loses the ability to walk or stand.
The current frontline treatment for Parkinson’s disease patients has remained much the same for the last 60 years. Levodopa, a chemical that is converted into dopamine in the brain, is used as a replacement therapy. It’s purpose is to replenish the dopamine that is continuously being lost for Parkinson’s disease patients. While levodopa treatment is effective in managing the symptoms seen in Parkinson’s disease, the benefits generally become less consistent over time. The drug is ultimately unable to slow down the disease progression. Commonly, as Parkinson’s disease progresses, patients will typically receive a combination of other medications in addition to levodopa. These include COMT, which mimics dopamine, or medications known as MAO-B inhibitors that slow the natural breakdown of dopamine.
For patients that either don’t respond, or stop responding to medication, there is a surgical procedure available. This treatment, called DBS or deep brain stimulation, is like inserting a “pacemaker” into the brain. The surgeon implants electrodes into the brain that will send electrical pulses to stimulate the firing of brain cells. Scientists have evidence that these electrical pulses serve to re-regulate the normal activation of brain cells that have been unregulated as a result of Parkinson’s disease, and that this ultimately helps to control disease symptoms. While this type of procedure is generally reserved for patients with advanced Parkinson’s disease, researchers have recently investigated whether DBS could be beneficial for early-stage Parkinson’s disease patients as well.
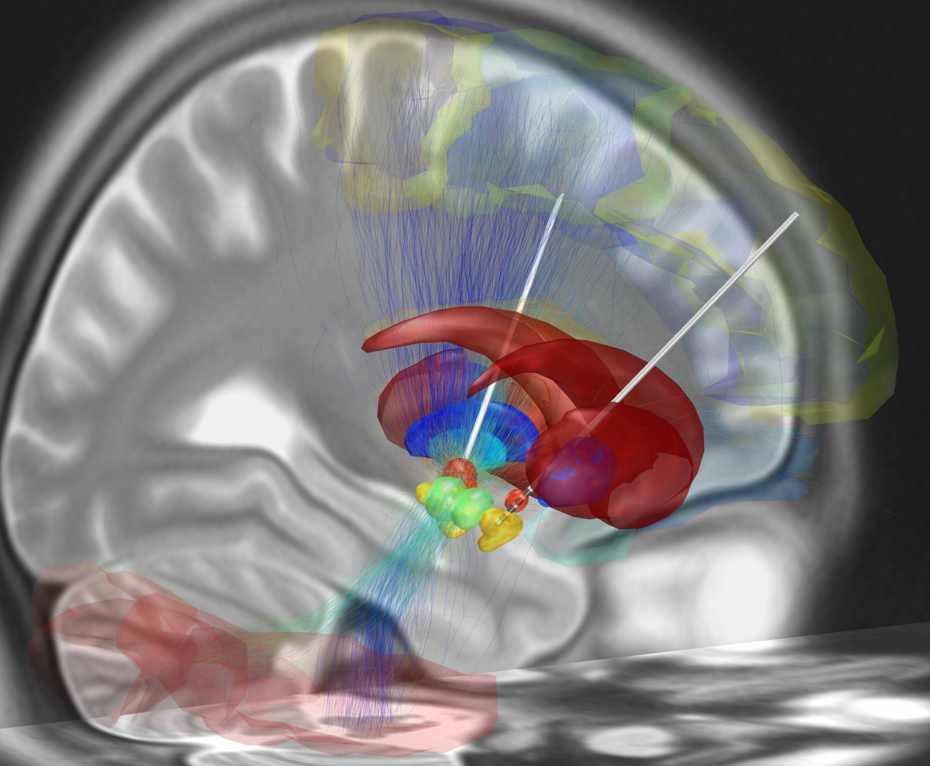
This is the location in the brain where the electrodes are placed for the DBS treatment. Andreashorn / CC BY-SA
At the Vanderbilt University Medical Center, scientists have completed a follow-up study to a pilot clinical trial in which early-stage Parkinson’s disease patients were given DBS in addition to their medication. These patients were compared to other early-stage patients that received only medication. The researchers looked at patient outcomes five years later, and found that the patients that received both medication and DBS fared much better on a variety of Parkinson’s disease outcome measures.
For example, the patients that received both DBS and medication were found to require much lower levodopa doses than early stage patients who did not undergo DBS. On average, patients that received both DBS and medication had an increase in their medication dose that was roughly half that of the patients that did not undergo DBS. They were also five times less likely to have a worsened resting tremor and were fifteen times less likely to need multiple types of Parkinson’s disease medications.
Taken together, the researchers concluded that early implementation of DBS may reduce the risk of Parkinson’s disease progression. If the results of future trials support these early results, the addition of DBS to early stage treatment of Parkinson’s disease may mean a better outcome and slower disease progression for patients. The researchers are now moving to a larger scale trial in order to more fully investigate the potential for DBS to slow Parkinson’s disease progression. If successful, this new treatment could be a landmark discovery for Parkinson’s disease care.

